Caring for someone with dementia can be challenging, and if they have a stoma, it can feel even more complex. Dementia is a condition that affects every person differently, and similarly, no two stomas are the same. This guide offers practical tips to help you support someone with both dementia and a stoma, whether they can manage their own care or need full assistance.
Understanding stomas
A stoma is an opening in the abdomen created by a surgeon to divert waste out of the body into a bag. This surgery is common and can affect anyone of any age for a variety of reasons, including bowel or bladder cancer. There are different types of stomas, and the three main ones are:
- Colostomy – outputs formed faeces from the colon (large intestine) into a closed bag which, when full, needs to be changed. This might only occur once or twice a day.
- Ileostomy – outputs looser faeces from the ileum (small intestine) into a drainable bag which, when full (several times a day), can be emptied into a toilet and remain in place until changed, usually once every 1-3 days.
- Urostomy – outputs urine into a urostomy bag which has a tap opening for emptying. This is drained frequently and changed about once every 1-3 days.
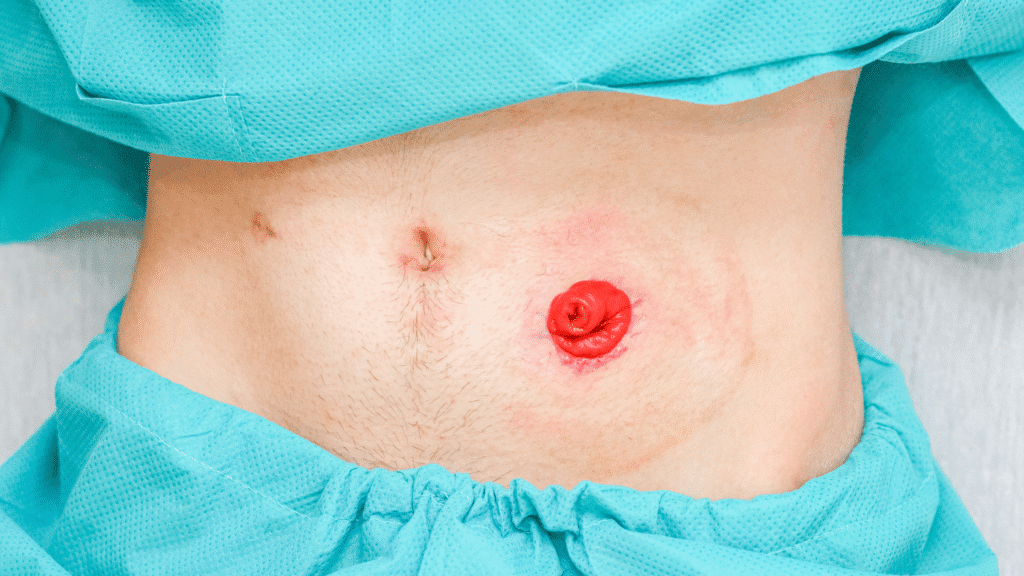
Understanding which type of stoma the person has is important to ensuring they get the right care.
Find out more: What is a stoma?
How dementia affects stoma care
Depending on the severity of their condition, a person with dementia may forget their stoma is there, become confused or distressed by it, or struggle to manage it. They might also become anxious and believe their appliance needs changing constantly, even when it doesn’t.
On the other hand, they may still be able to care for their own stoma. For example, if they had their stoma before the dementia developed, they may remember the sequence of changing their appliance. Attempts should be made to encourage their independence for as long as safely possible. Take into account any other conditions, like sight, hearing or dexterity impairments, that could impact their ability to look after it or take in instructions.
As dementia progresses, they may lose the ability to care for their stoma. It is best to prepare as much as possible for this eventuality.
If the person can care for their own stoma
Many people with a stoma who have dementia can maintain some independence with the right support and adaptations.
1. Simplify the process
Break down the process of changing their stoma bag into simple steps. You might need to repeat this a few times. Written instructions or diagrams may help – this Colostomy UK resource has step-by-step, visualised instructions. It might help to have these handy for a quick reminder of the correct sequence, such as stuck to the bathroom wall.
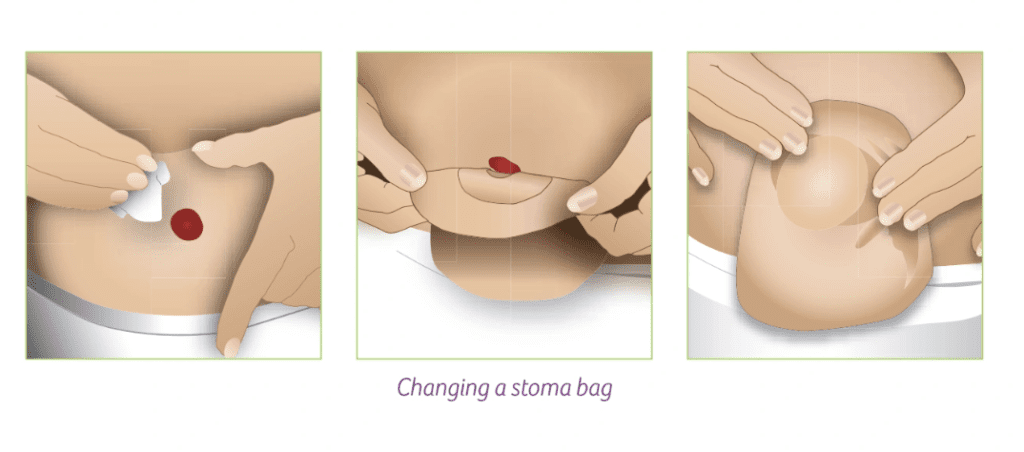
If their appliance is drainable (used for patients with an ileostomy or urostomy), ensure they are able to easily empty and reseal their pouch.
2. Create a calm environment
Encourage the patient to change their appliance in a quiet, calm and familiar environment, such as their bathroom. Remove unnecessary items from the bathroom to make it as simple as possible, with easy access to essential items like toilet paper and stoma supplies. A full-length mirror helps to make bag changes easier, as does plenty of space to lay out stoma supplies.
3. Prepare a stoma care kit
It may help to prepare stoma care kits for them, such as a small ziplock bag with all the tools needed for a single bag change. It might be useful to have lots of these in handy places, such as in the bathroom, by the bed and in the car. This might include:
- A fresh stoma appliance
- Medical adhesive remover for gently removing the appliance (wipes may be easier to use than spray cans)
- Dry wipes for cleaning the area of any output
- Any additional products as recommended by their stoma nurse, such as a stoma seal or barrier film (although keeping the process simple with as few steps as possible is advisable)
- Disposable gloves (this is optional but advisable for ensuring hygiene)
This can help them to keep their independence while reducing their mental load. This will also be handy for keeping any unexpected bag changes quick and simple. You might want to label these, for example, listing what they contain or the date they were made up.

4. Establish routines and reminders
Creating a routine for stoma care can be very helpful for dementia patients. For example, a diary or whiteboard to tick off when the stoma bag has been emptied or changed. Sticky notes can work well for timely reminders, such as with morning medication, next to the kettle or by the bed. Smart speakers may also be used to set digital prompts.
Gentle reassurance should help if they become anxious about their stoma pouch and want to change it too frequently. Redirecting their thoughts could also help, for example, by encouraging them to fill out a diary of when they last changed their bag and their diet, as well as any symptoms they experience.
If the person cannot care for their own stoma
As dementia progresses, you or other carers may need to take over the stoma care completely. Here are some strategies to make this easier.
1. Managing resistance to stoma bag help
The person with dementia may be resistant to help with their stoma. Distraction may help in this situation. For example, they could do another task, such as brushing their hair or cleaning their teeth, while the appliance is changed. Try to keep the process as quick as possible.
If you are unsure of how to change a stoma bag, this guide (available in print and digital formats) has step-by-step instructions for changing a stoma bag which can be applied to all types of pouches.

2. Positioning for stoma bag changes
Bag changes are best done while the person is standing, but if this is difficult, lying flat is another option. The key is choosing a position that provides a flat abdominal surface with good visibility. Sitting upright may cause folds or creases in the abdomen, which can make it hard for the appliance to adhere securely to the skin.
3. Monitoring the stoma
Stoma bags need emptying when they are approximately one-third to one-half full, which will change in frequency from person to person. A too-full bag is more likely to cause odour or leaks, and also feels heavy and uncomfortable, which can lead to the patient fiddling with it.
You might be able to note the timing and patterns of their stoma output so you can change/empty the bag promptly. Bowel stomas are likely to fill up soon after eating. Urostomy bags need to be emptied at about the same frequency that you would normally go to the bathroom to urinate.
4. Check skin health regularly
Check their peristomal skin at every change for any signs of irritation and keep an eye out for signs of discomfort such as itching. This way, you can address issues as soon as possible, before they escalate and become difficult to manage. Speak to a stoma nurse about any symptoms who can recommend action to take, which may be as simple as using a barrier film or checking the baseplate is being cut to the right size.
Read more: Peristomal skin protection
5. Preventing unwanted removal
Some people with dementia are restless, and this may lead to fiddling with their stoma bag, resulting in potential leaks. Firstly, check that the fiddling isn’t caused by soreness or discomfort, because peristomal skin can be sensitive (see above). In general, keeping them occupied with small tasks during the day should help to distract their attention away from the appliance. Sensory items or fidget toys may help.
Net pants may be useful (worn with normal underwear on top). You could also tuck their top into their pants to limit access to the appliance. Flange extenders with tapered edges may help to keep the appliance more secure and less likely to detach should any fiddling occur.
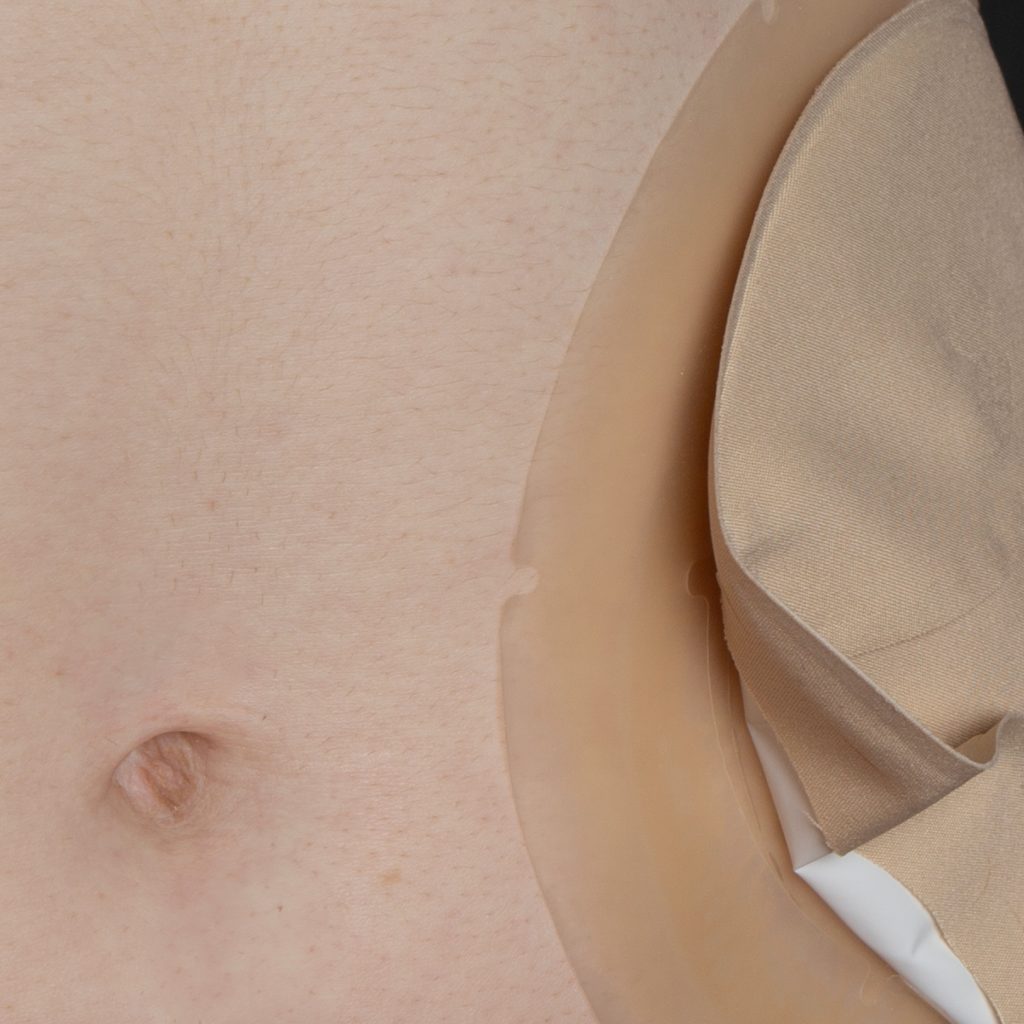
Some people with dementia may try to remove their stoma appliance at night. If this is the case, adaptive clothing may help, for example, a sleepsuit that is hard to remove. If you live with the person, a baby monitor can alert you to any nighttime movement. Any monitoring should be used in the least restrictive way possible and respect the person’s dignity and privacy. A waterproof mattress protector and dark sheets are commonly used by ostomates to mitigate the impact of nighttime leaks. Find out more: Sleeping with a stoma
Further general advice for caring for someone with dementia and a stoma
Organise stoma supplies
It may be helpful to set up a recurring order at regular intervals for their stoma supplies to be delivered, for example through a Dispensing Appliance Contractor (DAC). Through these services, you can request that their stoma appliances be precut to their stoma size. Just make sure that it is the correct size; stomas can change shape over time, and an appliance that is too large or too tight can lead to problems such as leaks and skin damage. Their stoma nurse can help with remeasuring if you are unsure.
Choose the right appliance
There are many different types of stoma pouches available, and choosing the right one is important. A one-piece appliance is generally simpler to apply for both carer and patient, with fewer steps involved when it comes to changing. However, a two-piece system might be more suitable if lots of changes are required. This is because the baseplate stays in place on the skin (for around three days usually) and the bag is detached, meaning less skin trauma and a simpler everyday process.

It is not normal to repeatedly suffer with stoma problems such as leaks, pancaking or skin irritation. If the person is struggling because of their stoma, contact their stoma care nurse. They can suggest techniques, products and treatments to help.
It’s okay to try different types of stoma bags until you find what works best for the person and their unique needs; there is no single brand or type that works best for everyone. Most stoma suppliers will be happy to help and can offer free samples. Read more: Ultimate guide to stoma bags
Medication considerations
The person may have had a large portion of their bowel removed during stoma surgery. People with dementia often take multiple medications, and altered absorption could affect both their dementia medications and other treatments. Speak to a medical professional about this either before or after surgery. This could be their stoma nurse, GP or surgeon.
The bowel also absorbs liquid, which means that drinking plenty is especially important for stoma patients. This Alzheimer’s Society post has advice on keeping dementia patients hydrated.
Bathroom adaptations
Making simple changes to the bathroom can reduce confusion and make stoma care safer:
- Leave the bathroom light on at night to make it easy to find.
- Removing the toilet lid or installing one that is a different colour to the rest of the toilet may reduce issues of forgetting to lift it and also make it easier to see.
- Remove bath mats if they create trip hazards.
- Keep the environment uncluttered with only essential items easily accessible.
Support for stoma patients with dementia
Try to involve dementia specialists and stoma care specialists in the care of the person. They are there to help you, and a holistic approach is always best. The person may be entitled to regular home visits to assist with stoma or dementia management.
If they live in a care home, talk to the staff and ensure they understand and feel comfortable helping the person with their stoma appliance. If they don’t, it might be possible to request a stoma nurse or training company go into the care home and provide stoma training for their staff.
Conclusion
Caring for someone with dementia and a stoma is challenging and requires patience and persistence. Remember that you don’t have to do this alone; professional support is available from a local stoma care team or healthcare professionals. There is also lots of reliable information online, and the resources below can help you access the specialist guidance you need.
Helpful resources
StoCare Stoma Advice and Support
Dementia UK (including a dementia helpline)
Colostomy UK (including a 24/7 stoma helpline)
Ileostomy and Internal Pouch Association
Although all our articles are written alongside qualified medical professionals, this information is for guidance only and does not replace the advice of healthcare professionals.